The 'inertia' of dementia care exposed by a tragedy
 PA Media
PA MediaA review into the case of an 88-year-old woman beaten to death by a fellow care home resident exposed a national "inertia" when it comes to dementia care. Despite being the leading cause of death in the UK, the condition has for years been without a government strategy for quality of care and skills, and we wait for a new policy to be implemented as part of NHS reforms. How have we been "conned" when it comes to dementia care and what has that meant for people living with the disease, and their families?
How was this brought to light?
 Family photo
Family photoIt is no secret that there is no overarching framework for dementia care in this country. Charities have long campaigned for improved standards and more support, pointing out that people with dementia and their families are left to navigate a confusing system after their initial diagnosis and as their condition progresses.
The extent of the national problem was laid bare when an Adult Safeguarding Review was published into the case of Sheila Hartman. In October 2022, a fellow resident of their Bedfordshire care home, 92-year-old Eunice Clarke, wandered from her room to Sheila's in the early hours. Believing Sheila was an intruder, Eunice beat her to death with her walking stick.
Both women were well-loved mothers with advanced dementia, the review heard.
The report's author, Dr Sheila Fish, found there was very little research around social care practice regarding bedroom doors in care homes, and said the tragedy revealed a "startling picture" and "apparent inertia" nationally around dementia.
"It brought the analogy of the emperor's new clothes to mind; the notion that we have been conned when it comes to dementia care, ripped off, but no-one is calling it out," she added.
She said a lack of a national dementia strategy or quality standards meant "expectations on [care home] providers are not clear or mandatory".
Sheila and Eunice became victims in a breakdown of arrangements which should have kept them safe, she added.
What does it mean for people with dementia?
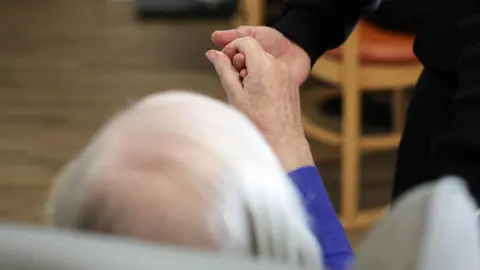 Reuters
ReutersAt the time of the incident - and to this day - there are no clear national standards for what "good" dementia support looks like, nor any mandated dementia training requirements for health and care staff.
Fish pointed out that this even included "what look like specialist dementia care homes or units".
She noted that the Care Quality Commission - which inspects care homes and care providers - began co-producing new guidance in 2024 but as yet there was no "robust" system to try to ensure quality, safety of environment or of care.
"It becomes easier to see how dementia care is not necessarily the specialist care you might expect for yourself or your loved ones," Fish said.
The Alzheimer's Society has repeatedly claimed that the barista making your flat white coffee has had more training than dementia care staff.
Last month, it said 50% of staff training packages contained just one to two hours on dementia, despite 70% of care home residents living with the condition.
The issue is a pressing one.
The charity estimated there were about 982,000 people with the condition in the UK and this was projected to rise to 1.4 million in 2040.
Unlike other conditions, there is no target in place to reduce the number of deaths. Diagnosis can be painfully slow, and breakthrough drugs are often too expensive for the NHS.
Dementia care falls under health, social care and the voluntary sector, so it can be unclear how to access help and support for some of the most vulnerable people in society - and who to hold to account when things go wrong.
Charlotte Lillford-Wildman, head of policy and public affairs at Dementia UK, said: "Dementia is the leading cause of death in the UK, yet too many people are left to navigate a fragmented and inconsistent system alone.
"Families often tell us that support after diagnosis is limited or short-term, with no clear point of contact.
"As a result, care is poorly organised and problems escalate until they reach crisis point."
In 2024, research by The Nuffield Foundation recommended the government take a more leading role in defining what "good" dementia care looks like, and take leadership on equipping staff to provide that care.
Baroness Casey, chairwoman of the independent commission on social care, has called for urgent action and strengthened national leadership on dementia.
How have we got here?
 PA Media
PA MediaDementia policy was centre-stage between 2009 and 2020.
The country's first dementia strategy was ushered in by Labour's Health Secretary Alan Johnson, under Prime Minister Gordon Brown. It was a five-year plan designed to promote better knowledge, ensure early diagnosis and support, and develop services to meet changing needs better.
In 2015, a further five-year plan was brought in. Conservative Prime Minister David Cameron described dementia as "one of the greatest challenges of our lifetime" and pledged more than £300m for research. There was a "serious intent" to prioritise dementia and to strive to make England the best country in the world for dementia care and support by 2020.
It expired in that Covid year, and since then policy has been marked by a "worrying inertia", Fish said, while the older population - and the number of dementia patients - increased.
Two years passed, and a 10-year plan was announced by subsequent Health Secretary Sajid Javid in 2022. It intended to improve outcomes for dementia and support people with their specific health and care needs.
However, the political turmoil and changing cast of characters in government meant it was dropped later that year. Instead of having its own focused plan, dementia was included, with cancer and mental health, in a Major Conditions Strategy.
It meant the UK was, in 2023, the only nation without a specific dementia strategy and specific funding, Fish said.
The strategy was paused - and remains unpublished - because the new Labour government commissioned Lord Darzi to investigate the state of the NHS, to inform a new 10-year plan of reform.
Published last year, it includes a Modern Service Framework (MSF) for frailty and dementia.
It has been billed to set standards for care and identify the best types of support that health professionals should provide.
Initially promised by spring 2026, it is now expected at the end of the year.
What is the new national strategy for dementia?
 Reuters
ReutersThe contents of the MSF are yet to be announced. The Department of Health and Social Care said it would drive "rapid and significant improvements in quality of care and productivity".
It would seek to reduce "unwarranted variation and narrow inequality" for those living with dementia, set national standards for dementia care and redirect NHS priorities to provide the best possible care and support.
"We know our health and adult social care system has struggled to support those with dementia, and we are committed to turning this around so every person living with the disease receives the high standard of care they need and deserve from diagnosis through to end of life," a department spokesperson said.
The Alzheimer's Society has called on the government to use the new framework to set an "ambitious goal" to reduce dementia deaths; ensure early and accurate diagnosis; support high-quality dementia training for the social care workforce and prepare the NHS to deliver new treatments, as they become available.
Lillford-Wildman, for Dementia UK, said it was an important opportunity for real progress in joining up and improving dementia care.
"It must focus on how care is delivered day to day," she stressed.
"That means ensuring ongoing, co-ordinated support, clear accountability, and a more proactive approach to managing people's needs as they change over time."
Do you have a story suggestion? Contact us below.
Follow East of England news on X, Instagram and Facebook: BBC Beds, Herts & Bucks, BBC Cambridgeshire, BBC Essex, BBC Norfolk, BBC Northamptonshire or BBC Suffolk.
